Tips for Before and After an Ablation to Improve Odds of Success

The prospect of an atrial fibrillation / Afib ablation procedure can feel daunting, especially if this is your first major interventional procedure. But let’s get right to it: cardiac catheter ablations are very safe, effective (in the properly selected patient), and do not require significant downtime after the procedure. They are also excellent options because they do not preclude other therapies, like medication if you need additional treatment to address a particularly stubborn arrhythmia.
Is Afib Dangerous?

If you’ve recently experienced your first atrial fibrillation or Afib episode, it may have been a scary experience, and you will likely be asking yourself if Afib is, in fact, dangerous. After all, if the attack was relatively strong, it’s hard to think anything less than “absolutely, it is dangerous!” However, the answer to this question is less straightforward than you think. Yes, the mechanics of Afib puts a significant strain on your heart, but your heart is also a very resilient muscle, and there are plenty of other factors that will affect how your body ultimately handles the condition now and in the future.
Comparing Traditional Pacemakers to Leadless Pacemakers. Is One Better?
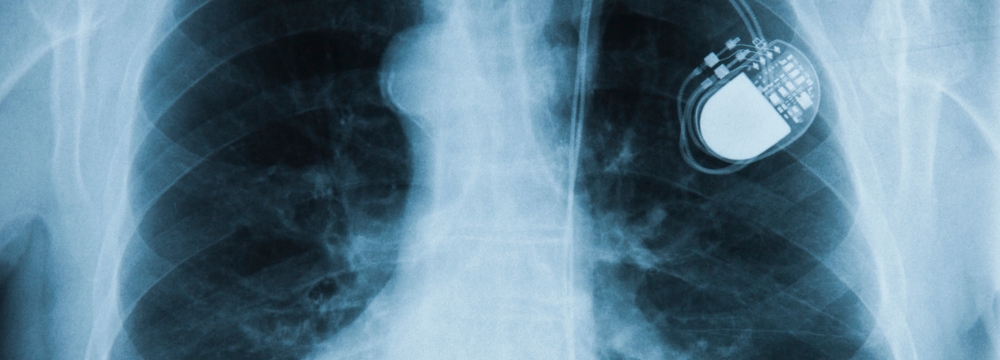
For decades, traditional pacemakers have been the gold standard in heart-pacing for bradycardia, also known as a slow heartbeat. This involves placing a small battery, known as a pulse generator, under a flap of skin in the chest muscle and connecting it to the heart with physical wires or leads. These pacemakers are very effective, but as with many things in the field of cardiology and electrophysiology, there is room for improvement. In our field especially, there is a significant technological and clinical push behind innovations and improvement of devices and techniques.
The result has been newer technology in the form of wireless or leadless pacemakers. These pacemakers are fully self-contained and attached to the heart’s ventricle, meaning they do not need wires to deliver their electrical impulses.
Comparing Cardiac Catheter Ablation Success During Paroxysmal Versus Persistent and Long-Standing Persistent Afib
When we diagnose patients with Afib, we must discuss the difference between varying stages of the condition, as this can be significant in the decision-making continuum. Before we get into the success rates of cardiac catheter ablation between stages of Afib, it is essential that we define the progression of the condition and how it manifests in the patient.
In most cases, Afib begins as occasional or paroxysmal. This broadly means patients experience a couple of episodes, lasting for 30 seconds or more but ending rapidly (within seconds, hours, or even a couple of days), in a week. Because it is occasional, many patients wait too long to see an electrophysiologist. Or they visit their primary care physician or general cardiologist for an EKG. Yet often, this EKG shows nothing wrong because paroxysmal Afib episodes are irregular and unpredictable. EKGs only offer a snapshot of the heart during the office visit. The result is that many patients are sent home without a definitive diagnosis.
What Can I Do to Naturally Prevent Atrial Fibrillation

Atrial fibrillation, or Afib, is the most common arrhythmia in the United States and is estimated to affect upwards of 5 million Americans. Every year a greater number of patients are diagnosed with this condition because of several factors. While there are a few non-modifiable factors – those that cannot be helped (like age and genetics), we can go a long way in reducing the likelihood of developing Afib by making simple but meaningful lifestyle changes. Unfortunately, many of us have developed bad heart health habits over the course of years or even our entire lifetime, so while straightforward, we understand how difficult these changes can be to implement.
Artificial Intelligence in the Treatment of Atrial Fibrillation & Other Arrhythmias

By now, we’ve all seen the incredible technological advances modern society has made. While we routinely see new devices on the market in medicine, especially in electrophysiology, our specialty, in particular, relies on advanced software to map the heart, guide the catheter, identify treatment areas and ultimately evaluate the effectiveness of the ablation or other arrhythmia treatment.
Currently, the technology we use relies on our best judgment to identify where the arrhythmia originates and ultimately treat the appropriate areas during an ablation. Once the treatment has been completed, we use the same technology to evaluate whether the treatment has been successful.
Exciting Leadless Pacemaker Technology on the Horizon
Pacemakers have been the gold standard in treating slow heart rhythms known as bradycardia for decades. Most of us know someone with a pacemaker. This tiny device offers patients a life-changing and lifestyle-restoring option for what would otherwise be a debilitating and chronic condition like congestive heart failure. Implanted in a very safe and straightforward procedure, traditional pacemakers have few risks. However, one of the most significant concerns of a conventional pacemaker is the malfunction or breakage of the wires that connect the pulse generator/battery to the heart itself. Further, while traditional pacemaker technology has improved to the degree that they are smaller than ever, it still requires a bulky implant under the skin.
Artificial Sweeteners vs. Sugar – Which Is Better for Your Heart

Regarding lifestyle issues and the heart, metabolic disease and obesity are some of the most concerning issues we, as cardiologists, face. While the specialty of cardiology and subspecialty of electrophysiology have made leaps and bounds over the years, the treatment of many cardiovascular concerns is hampered by our decidedly less healthy society. We’ve seen a rise in cardiovascular problems in ever younger patients, and irregular heart rhythms are becoming more common. Certain arrhythmias like atrial fibrillation or Afib come with some severe potential follow-on consequences, not least of which is a five times increased risk of stroke and a significantly increased risk of heart attack or congestive heart failure.
Could Your Chronic Fatigue Be a Result of a Cardiac Arrhythmia?

Cardiac arrhythmias can vary dramatically in their presentation, frequency, intensity, and symptoms. Electrophysiologists like Dr. Tordini see heartbeat irregularities ranging from very slow to extremely fast. While cardiac arrhythmias have been a concern since the dawn of humanity, they have become decidedly worse in recent decades as our overall health, and our hearts have declined.
When we think of cardiac arrhythmia, our minds may think of a racing heart and other standard symptoms. These should not be discounted by any means. However, these heart palpitations, flutters, and feelings of pounding in the chest are not the only symptoms that arrhythmia patients will feel. Chronic fatigue is a widespread concern associated with some fast and alternately slow heartbeats. The diagnosis is made even more challenging to diagnose when patients suffer from, for example, silent atrial fibrillation or Afib. When diagnosing chronic fatigue, the possibility of arrhythmia, especially one that does not have outward symptoms, may not be top of mind for most medical professionals.
When Chest Pain Becomes a Problem – What to Do

Let’s get right to it and say that while chest pain, known as angina, can have many causes, it should never be ignored due to the possibility of it being a precursor for severe cardiovascular events. As such, if you are experiencing a medical emergency, be sure to dial 911 immediately or get to your nearest emergency room. If you have a non-emergent, persistent chest pain that cannot be explained away, be sure to visit your primary care specialist or cardiologist urgently to have it evaluated. Let’s explore some of the non-cardiac-related chest pain many of us will experience: